Methods:
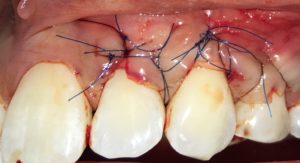
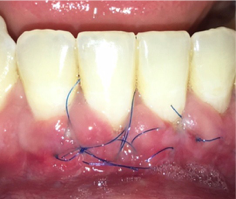
Forty-seven patients with 64 sites with lack of attached gingiva were treated with free gingival grafts and 64 control sites were left untreated. Patients were recalled every 4 to 6 months. Gingival recession depth, keratinized tissue width, and probing depth were measured at baseline and extending to the follow up period (18 to 35 years)
Results:
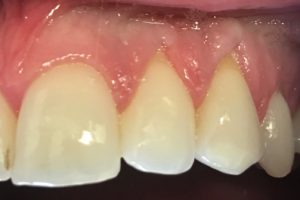
At the end of the follow up period, 83% of the 64 treated sites showed recession reduction whereas 48% of the 64 untreated sites experienced increase in recession. Treated sites ended with gingival margin 1.7 mm more coronal and keratinized tissue 3.3 mm wider than untreated sites.
Conclusions:
Sites treated with gingival augmentation procedures resulted in coronal displacement of the gingival margin and reduced recession, whereas the contralateral untreated sites showed a tendency for increased recession and a tendency to develop new recession during the 18 to 3 year follow up.
For more information please refer to:
Journal of Periodontology 2009 Sep;80(9):1399-405
Periodontal conditions of sites treated with gingival augmentation surgery compared to untreated contralateral homologous sites: a 10- to 27-year long-term study.
Agudio G1, Nieri M, Rotundo R, Franceschi D, Cortellini P, Pini Prato GP.